Best Affordable EMR for Small Therapy Practices: Cost-Effective Solutions for Efficient Patient Care
Looking for the best affordable EMR for small therapy practices? Discover cost-effective solutions that streamline documentation, improve patient care, and maximize your clinic’s ROI. Learn how HelloNote’s cloud-based, all-in-one system offers transparent pricing, easy adoption, and features tailored specifically for physical, occupational, and speech-language therapy practices. Make the smart choice for your clinic today!

Implementing an Electronic Medical Record (EMR) system is a critical step for healthcare organizations looking to improve efficiency, streamline documentation, and enhance patient care. However, the cost of EMR implementation and maintenance can be a major concern, especially for small and mid-sized practices operating on tight budgets.
From software and hardware expenses to training and ongoing support, managing the financial impact of an EMR system requires careful planning and strategic decision-making. In this article, we’ll explore the key costs associated with EMR implementation, discuss cost-saving strategies, and highlight how practices can maximize their return on investment (ROI) while ensuring a smooth and successful transition.
Understanding the Costs of EMR Implementation
EMR costs extend beyond just the initial purchase price. A comprehensive budget should include:
1. Upfront Costs (Initial Investment)
-
- Software Licensing Fees: Costs depend on whether the EMR is a cloud-based subscription (SaaS) or on-premise software that requires a one-time purchase.
-
- Hardware Costs: May include computers, tablets, servers, and networking infrastructure for clinics that require on-site hosting.
-
- Implementation & Setup: Covers system configuration, data migration from previous records, and integration with existing systems (billing, scheduling, or telehealth platforms).
2. Training and Onboarding Costs
-
- Staff Training Sessions: Providers and administrative staff must learn how to use the system efficiently.
-
- Product Support During Transition: Some vendors offer free support, while others charge for ongoing implementation assistance.
-
- Time Investment: Initial product adoption may slow down clinic operations temporarily, affecting patient volume and revenue.
3. Ongoing Costs (Maintenance & Support)
-
- Subscription Fees for Cloud-Based EMRs: Monthly or annual costs that include software updates, security patches, and support.
-
- IT Support & Maintenance: Practices using on-premise EMRs must budget for IT professionals to manage servers and security protocols.
-
- Compliance & Security Upgrades: Ensuring that the EMR remains HIPAA-compliant and updated with the latest healthcare regulations.
4. Hidden Costs to Consider
-
- Customization Fees: Some EMRs charge extra for specialized templates or custom reporting features.
-
- Data Storage & Backup Costs: Especially for image-heavy practices like radiology or therapy clinics using video-based documentation.
-
- Downtime & Productivity Losses: Transitioning to a new EMR can initially disrupt workflows, impacting revenue until staff become proficient.
Cost-Saving Strategies for EMR Implementation
While EMR adoption can be costly, small and mid-sized practices can implement smart cost-management strategies to minimize expenses without compromising quality.
1. Choosing the Right EMR for Your Practice Size
-
- Cloud-Based EMRs Reduce Upfront Costs: Unlike on-premise solutions, cloud-based EMRs eliminate the need for costly hardware installations and IT maintenance.
-
- Scalable Pricing Plans: Many vendors offer tiered pricing based on practice size, allowing small clinics to pay for only what they need.
-
- Therapy-Specific EMRs: Specialized platforms (like HelloNote for PT, OT, and SLPs) prevent unnecessary spending on irrelevant features.
2. Taking Advantage of Government Incentives
-
- Medicare & Medicaid Incentive Programs: The Promoting Interoperability Program (formerly Meaningful Use) offers financial incentives for eligible providers who implement certified EMRs.
-
- Tax Deductions for Software & IT Upgrades: Many practices can write off EMR-related expenses under business technology deductions.
3. Optimizing Training & Staff Adoption
-
- Choose an EMR with Intuitive UX: A user-friendly EMR reduces training time and mistakes, lowering long-term costs.
-
- Vendor-Supported Training: Look for EMRs that offer free training sessions, live demos, or online resources to minimize additional costs.
-
- Gradual Implementation: Rolling out the EMR in phases rather than all at once can help staff adjust without overwhelming workflows.
4. Reducing Ongoing Maintenance Expenses
-
- Opt for All-in-One Solutions: Choosing an integrated EMR with built-in billing, scheduling, and telehealth eliminates the need for multiple software subscriptions.
-
- Ensure Vendor Support Is Included: Some EMRs charge extra for technical support, so practices should confirm upfront if customer service is included in the cost.
-
- Regular System Audits: Reviewing billing reports, claim rejections, and documentation efficiency helps prevent costly errors and revenue loss.
Maximizing ROI: Ensuring Long-Term Value from Your EMR
Instead of focusing solely on cost-cutting, clinics should evaluate EMRs based on long-term value. A well-implemented EMR can:
-
- Increase Efficiency: Automated workflows reduce manual data entry and minimize administrative burdens.
-
- Improve Revenue Cycle Management: Built-in billing tools and claims tracking ensure faster reimbursements and fewer denials.
-
- Enhance Patient Retention: Features like patient portals, telehealth, and automated appointment reminders improve engagement and retention.
-
- Strengthen Compliance & Reduce Risk: Ensuring HIPAA compliance, accurate documentation, and proper coding prevents penalties and audits.
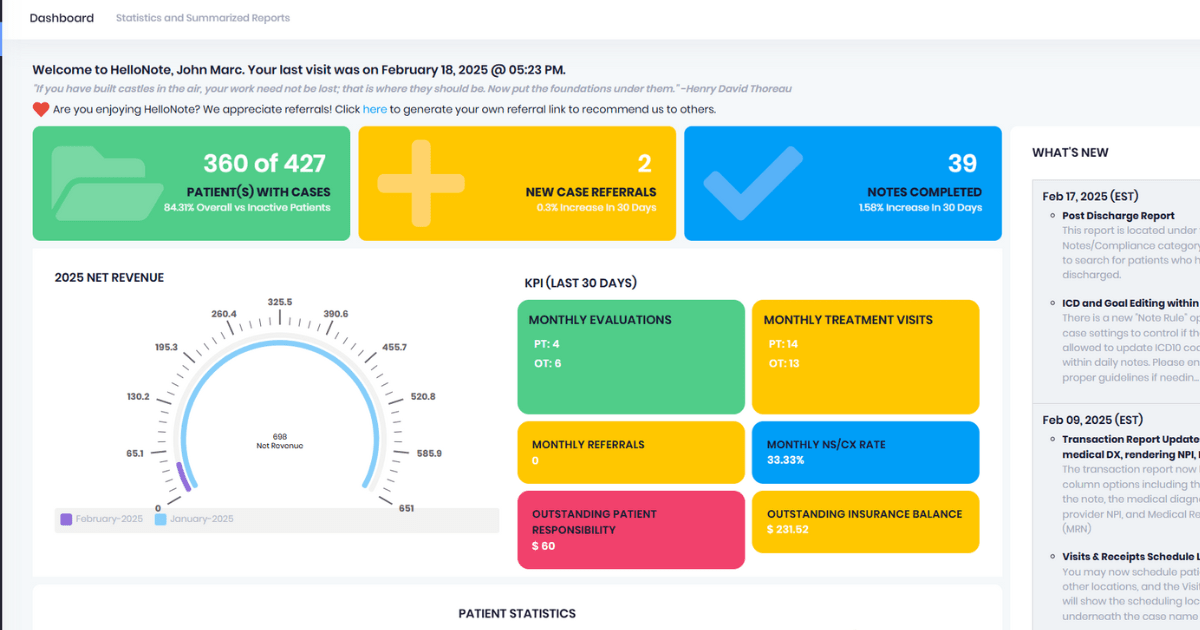
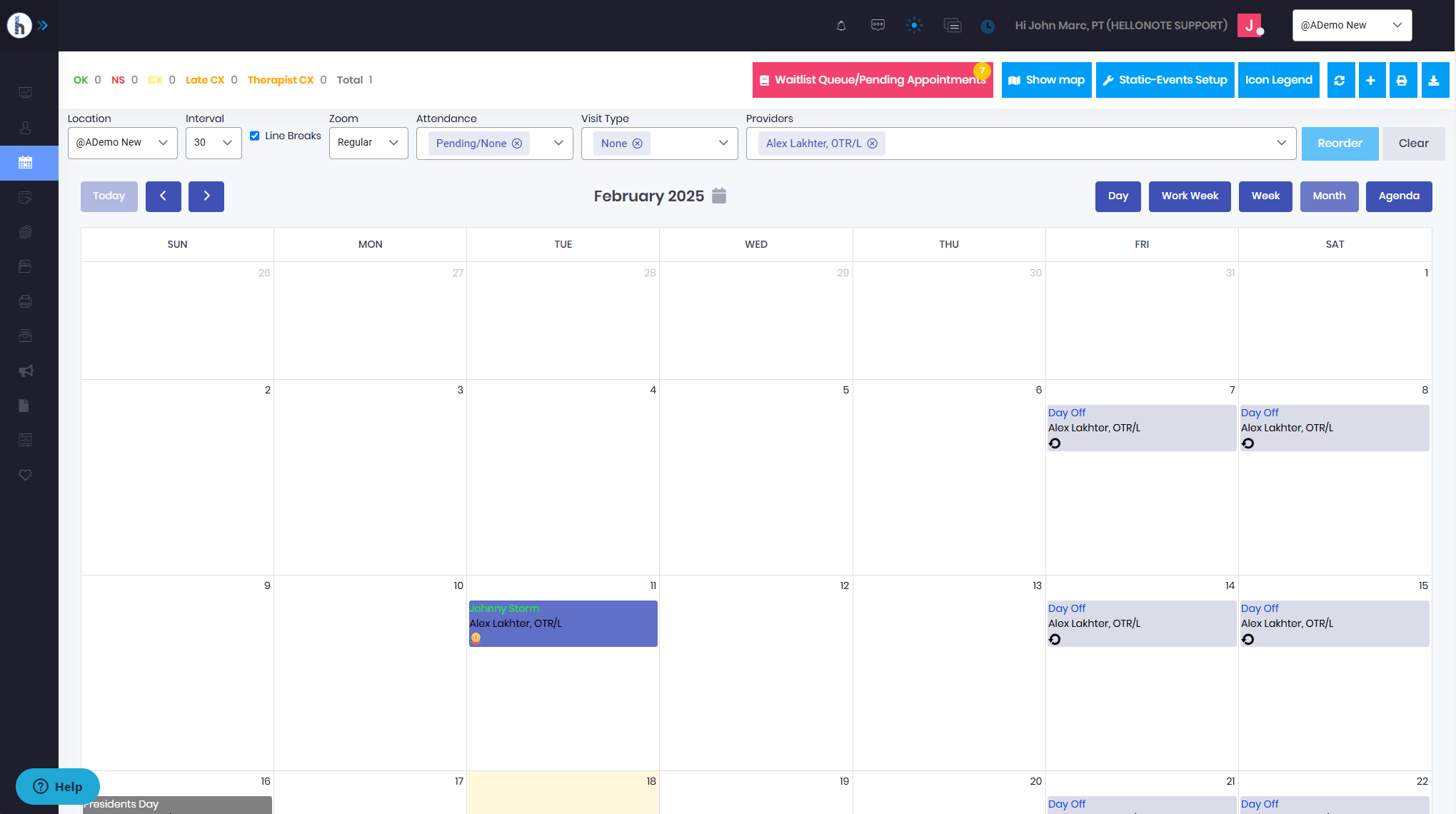
How HelloNote Helps Small & Mid-Sized Practices Manage EMR Costs
At HelloNote, we understand that small and mid-sized therapy clinics require affordable, feature-rich EMRs without hidden costs. That’s why we offer a solution designed to optimize your clinic’s budget while meeting the unique needs of physical, occupational, and speech-language pathologists.
Here’s how HelloNote supports cost-effective EMR management:
- Transparent Pricing with No Hidden Fees: Flexible subscription plans tailored to your clinic’s size and budget, with no unexpected charges. We believe in honest, straightforward pricing, so you know exactly what you’re paying for without any surprises.
- All-in-One EMR with Built-In Billing & Scheduling: Streamline your clinic operations with an integrated system that combines billing, scheduling, and documentation. Avoid additional costs for third-party software integrations that other platforms may require.
- Cloud-Based Platform with No Hardware Expenses: Secure, HIPAA-compliant cloud storage means you don’t have to worry about expensive IT infrastructure or ongoing maintenance. Scalable to your needs, so you only pay for what you use and can expand as your practice grows.
- Free Live Training & Customer Support: Onboarding made simple with free live training sessions, so your staff can get up to speed quickly. Ongoing support at no additional cost, ensuring that you always have assistance when needed.
- Customizable Features for Therapy Workflows: Prebuilt templates designed for PT, OT, and SLP practices, making documentation efficient and compliant. Outcome tracking and compliance tools that simplify reporting and ensure you stay on top of regulatory requirements.
- Easy-to-Use Platform with Integrated Tutorials: HelloNote is designed with therapists in mind, offering an intuitive interface that minimizes the learning curve. Integrated video tutorials walk you through every step, from creating patient records to completing detailed therapy notes, ensuring you don’t need extra training resources. Step-by-step guides within the platform help your team navigate the system smoothly, so your practice can hit the ground running with minimal disruption.
Why Choose HelloNote?
Looking for an EMR system that combines affordability, functionality, and ease of use? HelloNote is the solution for your practice. With our all-in-one system, transparent pricing, and integrated tutorials, we provide everything you need to run your clinic efficiently and cost-effectively.
Smart Cost Management for EMR Success
Implementing an EMR doesn’t have to break the bank—with the right planning, strategic choices, and vendor support, clinics can reduce costs while maximizing efficiency and compliance.
Key Takeaways:
-
- Understanding the full cost of EMR implementation helps avoid unexpected expenses.
-
- Choosing the right EMR based on practice size ensures cost efficiency.
-
- Leveraging government incentives and training resources reduces upfront and ongoing costs.
-
- Investing in an EMR that improves billing, scheduling, and compliance leads to long-term financial success.
By selecting an EMR that aligns with your practice’s needs, you can improve patient care, boost profitability, and future-proof your clinic—without the financial strain.